Increased federal focus on accelerating AI research has augmented interest and opportunities to support healthy living and aging across the life course using AI-assisted health monitoring, disease prediction, and caregiver supports. The current, and growing, shortfall of unpaid and paid caregivers underlines the need for technological solutions that increase caregiver capacity and reduce care needs by preserving health and independence as people age. To ensure these technologies reach the populations that they could most benefit, efficient commercialization, regulation, and reimbursement pathways for AgeTech solutions are needed.
On March 19–20, 2026, the a2 Collective, a research program funded by the National Institute on Aging (NIA), convened its fourth annual a2 National Symposium to discuss progress, opportunities, and challenges in the design, implementation, evaluation, and commercialization of AI and other emerging technologies for healthy aging and caregiver support. The a2 Collective represents the Artificial Intelligence and Technology Collaboratories (AITC) for Aging Research program, through which NIA has awarded more than $40M over a 5-year period to technology development projects with the potential to improve the lives of older adults, including individuals with Alzheimer’s disease and related dementias (AD/ADRD), and their caregivers. The symposium planning was led by the a2 Collective Coordinating Center, co-hosted by the Johns Hopkins University Carey Business School, and held at the Hopkins Bloomberg Center in Washington, D.C. with over 200 in-person attendees and nearly 50 virtual participants.
AI to advance federal health priorities: supporting federal research and the development of digital health reimbursement and regulatory pathways
In response to the boom in AI-supported technology across the health and aging fields, the U.S. Department of Health and Human Services (HHS) has been working to establish clear pathways to utilize AI to improve Americans’ health across the lifespan.
In a fireside chat moderated by Arman Sharma, HHS Deputy Chief AI Officer, members of HHS leadership discussed how the technologies developed by a2 pilot awardees fit within the current HHS policy landscape. Mary Lazare, MS, MA, Administration for Community Living, discussed the agency’s Caregiver Artificial Intelligence Prize Challenge, which aims to address the current and projected shortfall of paid and unpaid caregivers for older adults and adults with disabilities by soliciting tools that leverage AI to improve caregiver productivity, increasing the capacity of the current workforce. Lazare and Thomas Keane, MD, MBA, Assistant Secretary for Technology Policy and National Coordinator for Health Information Technology, agreed that deployment-ready AI tools must be sufficiently trustworthy that providers believe the technology will help them and not harm patients, securely store and use patient data, and have a measurable return on investment by improving patients’ health outcomes or saving doctors’ time.

In a panel discussion on how various HHS agencies are interacting with AI, Nora Connor, PhD, Centers for Medicare & Medicaid Services Innovation Center (CMMI), described how CMMI’s Advancing Chronic Care with Effective, Scalable Solutions (ACCESS) Model incentivizes the use of digital health solutions by offering payments tied to specific patient outcomes, which can be achieved using digital health tools, rather than payments in return for services rendered. Demand for these digital health tools dramatically increased once payments began. Michael A. Morgan, PhD, U.S. Food and Drug Administration (FDA), recounted how the FDA created Elsa (short for “Electronic Language System Assistant”), an internal generative AI tool that helps employees with administrative tasks. The FDA has embraced AI to increase their operational efficiency, with Elsa having a reported 70% adoption rate across the agency. Rafid Fadul, MD, MBA, Advanced Research Projects Agency for Health (ARPA-H), reported that all of ARPA-H’s programs incorporate AI in some capacity, highlighting the clinical AI agent regulatory pathway that their Agentic AI-Enabled Cardiovascular Care Transformation project is co-developing with the FDA. Concurrently with recognizing AI’s potential to improve outcomes for patients across the life course, HHS is attending closely to implementation challenges such as reimbursement, regulation, and ensuring patient privacy and safety.
Using AI to identify predictive biomarkers of aging
The potential utility of aging and AD/ADRD biomarkers was commonly discussed throughout the symposium. Acknowledging the varied uses of the term in scientific and HealthTech discourse, Luigi Ferrucci, MD, PhD, NIA, asked his panelists to share how they define biomarkers. The panel agreed that biomarkers are measurements that correlate with some sort of functional health change. Vadim Gladyshev, PhD, Harvard Medical School, identified that much confusion regarding biomarkers of aging can be attributed to differing definitions of what “aging” actually is (e.g., demographic age, likelihood of dying tomorrow, functional or cognitive decline). Peter Abadir, MD, Johns Hopkins University, suggested frailty as a meaningful biomarker of aging, due to its correlation with a person’s whole system biology. David Glass, MD, Regeneron Pharmaceuticals, emphasized that a useful biomarker is one that can be therapeutically addressed (i.e., treating frailty through a medication that increases muscle mass) and suggested that AI models could identify digital biomarkers within the large longitudinal datasets generated by wearables.
The utility of this type of longitudinal data was described by Rosalind Picard, ScD, MIT Media Lab and Empatica, in her presentation on how EpiMonitor, a watch containing an electrodermal sensor, can detect seizures using an FDA-cleared AI algorithm, alerting the patient’s caregiver and updating their seizure record, which is used by their physician to adapt their treatment plan. This type of monitoring is vital for any patient with epilepsy, and in older adults especially, since some types of seizures can be mistaken for other conditions more common in older adults (e.g., dementia, cardiac arrhythmia, syncope).

More than 60 investigators funded in the fourth and fifth a2 Pilot Awards cohorts presented their work during poster and technology demo sessions, many of which focused on identifying novel digital biomarkers. As examples, projects presented by Vineet Raghu, PhD, Massachusetts General Hospital, and Tianyi Ren, PhD, KurtLab at the University of Washington, used AI to find biomarkers of aging and cognitive impairment, respectively, from MRI imaging. Vijaya Kolachalama, PhD, Boston University, demonstrated how Cognimark, an AI tool integrated into an electronic health record (EHR) system, flags patients with possible mild cognitive impairment (MCI) or dementia based on all available patient data and provides the physician with a report on what aspects of the patient’s data caused the flag. Dr. Kolachalama’s team has piloted the technology in multiple clinics, covering over 100,000 patients, and will soon be expanding to cover about 7 million patients across several states through a new grant. Both in a poster and as part of the a2 Collective x AgeTech CollaborativeTM from AARP Pitch Challenge, Nili Solomonov, PhD, and Logan Grosenick, PhD, both of Weill Cornell Medicine, discussed how their SOCIAL-Q platform can analyze a brief conversation with an older adult using AI to identify whether a person is experiencing social disconnection, characterize the type of disconnection, and match them with appropriate social support.
Commercialization of AgeTech
The unique challenges and considerations associated with commercializing AgeTech solutions were a prominent theme throughout the symposium. As the creator of the first FDA-cleared digital therapeutic, BlueStar, Anand Iyer, PhD, MBA, Welldoc, encouraged HealthTech startups to pursue FDA clearance as a medical device and then partner with large, industry-leading companies on wellness devices, rather than compete with tech giants in the wellness space. Dr. Iyer stressed that AI tools shouldn’t be used to replace physicians; rather, they should expand healthcare providers’ capacity by handling low-risk tasks.
In a panel discussion moderated by Todd Haim, PhD, NIA, a2 Pilot Awards alumni shared that the most rewarding or “fun” aspect of commercialization is seeing a patient get to actually use their products. However, panelists Anna Barnacka, PhD, MindMics; Kunal Parikh, PhD, Johns Hopkins University and Visilant; Kyle Rand, Rendever; and Randall Williams, MD, WellSaid AI, agreed that the easiest place to make mistakes along the commercialization pathway lies in decision-making about which people to work with—whether as external partners or within the organization. David Yonce, MS, MBA, Cogwear, along with the rest of the panelists, stressed the importance of flexibility and the ability to pivot a startup’s direction to respond to unmet need.


The future of AI to support healthy aging
The symposium showcased the cutting edge of current AI-supported AgeTech and projected how AI might become more integrated into the care of older adults in the future. During a panel discussion on AI’s role in the next decade, Hon Pak, MD, MBA, Samsung Electronics, identified that AI could help support the increasingly overloaded workforce of caregivers. Russell Taylor, PhD, Johns Hopkins University, made a similar point in his own presentation, discussing how AI-enabled robotics can and do supplement healthcare workers’ ability and efficiency in areas ranging from the operating room to home health care. Multiple a2 pilot awardees are developing robotic supports for caregiving. As examples, Kruthika Gangaraju, Worcester Polytechnic Institute, presented a poster on a smart robot that could assist adults who experience memory challenges with activities of daily living, and Nilanjan Chakraborty, PhD, Stony Brook University, presented a poster on a robotic system that would allow a caregiver to use hand-over-hand guidance to teach a robot how to complete care tasks.
In the panel on AI’s role in the next decade, Sudeshna Das, PhD, Harvard Medical School, noted that current dementia diagnoses happen too late for patients to benefit from most preventative treatments and suggested that AI could facilitate earlier disease detection or prediction for patients. In the future, computation-heavy AI disease prediction tools may benefit from quantum computing technologies, whose unique mechanics allow for faster and different computing than current binary computing, as explained by Matthew Versaggi, MS, MBA, White House Presidential Innovation Fellow in AI, in his presentation on the topic.
As federal representatives participating in the panel discussion on AI’s role in the next decade, Shari Ling, MD, Centers for Medicare & Medicaid Services, and Anindita Saha, FDA, emphasized the need for the developers of future health tools to resist building their solutions in silos. Patients will manage multiple conditions across the life course, often concurrently, and solutions should be able to work across condition types. Furthermore, establishing meaningful, industry-wide, and patient-informed health outcomes will facilitate the distribution, regulation, and reimbursement of digital health tools.
In a session focused on the future of digitally enhanced dementia diagnostics and therapeutics, Jason Karlawish, MD, University of Pennsylvania, and I. Glenn Cohen, JD, Harvard Law School, discussed key ethical considerations relevant to many of the technologies presented across the symposium’s sessions, including:

• A shift in individuals’ agency regarding the collection of their data is occurring, moving from individuals actively deciding to provide an AI tool with their personal data for a specific purpose to the passive incorporation of individuals’ data into AI models.
• If a device does not have a built-in physical limitation on what data are collected, the default market inclination will be for increasing amounts of data to be collected.
• While health monitoring seems benevolent, AgeTech developers and the caregivers who choose to use an AI product must consider how much consent a patient with dementia has given to be constantly surveilled.
• Current health data privacy laws (e.g., HIPAA) focus on the covered entities and who must comply but may be inadequate for non-health data that can be used to make health inferences.
• No legal protection model currently exists for individuals who are predicted to develop dementia but have not yet experienced significant cognitive decline, so predictive technology could impact older adults’ autonomy (e.g., employment or driver’s license status) in the future.
• Care planning should include asking about a person’s preferences regarding AI monitoring and support.
By encouraging a2 pilot awardees to consider both the effectiveness and the ethical and legal ramifications of their AgeTech solutions, speakers across the symposium advocated for AI innovation that promotes safe and healthy living across the lifespan. The a2 National Symposium highlighted the importance of maintaining focus on older adults, who are at the forefront of utilizing AI solutions to support health and independence, creating momentum that will lead to positive ripple effects for all individuals as they age.

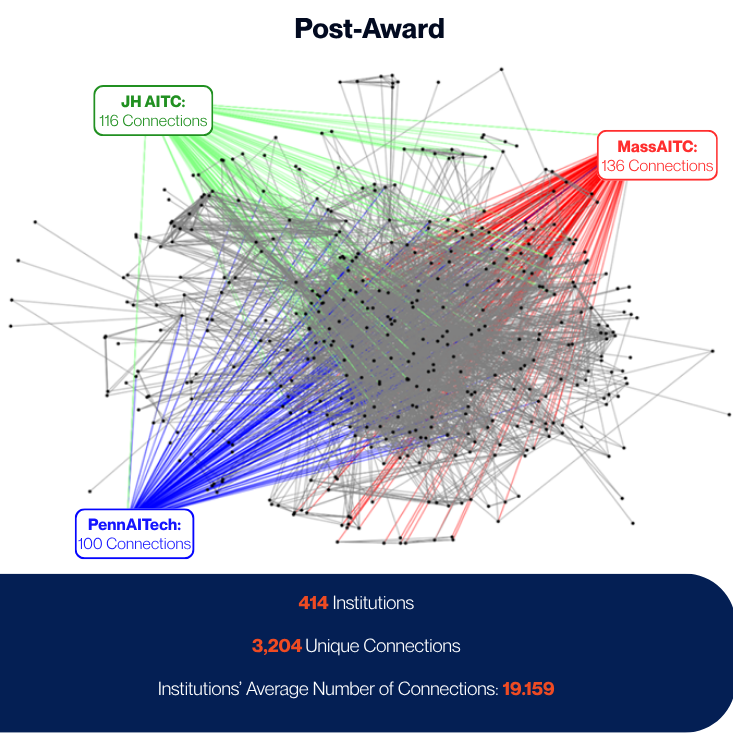
NIA is one of 27 Institutes and Centers of the National Institutes of Health at the U.S. Department of Health and Human Services. The a2 Collective is funded through NIA grants U24AG073094 (the a2 Collective Coordinating Center), P30AG073104 (JH AITC), P30AG073105 (PennAITech), and P30AG073107 (MassAITC).
The full 2026 a2 National Symposium agenda and video recordings of plenary sessions, along with upcoming events, additional resources, and other information, are available via the a2 Collective website. You can also follow the a2 Collective’s work on LinkedIn.